An Archways Magazine Interview with Sr. Mary Catherine Redmond PBVM
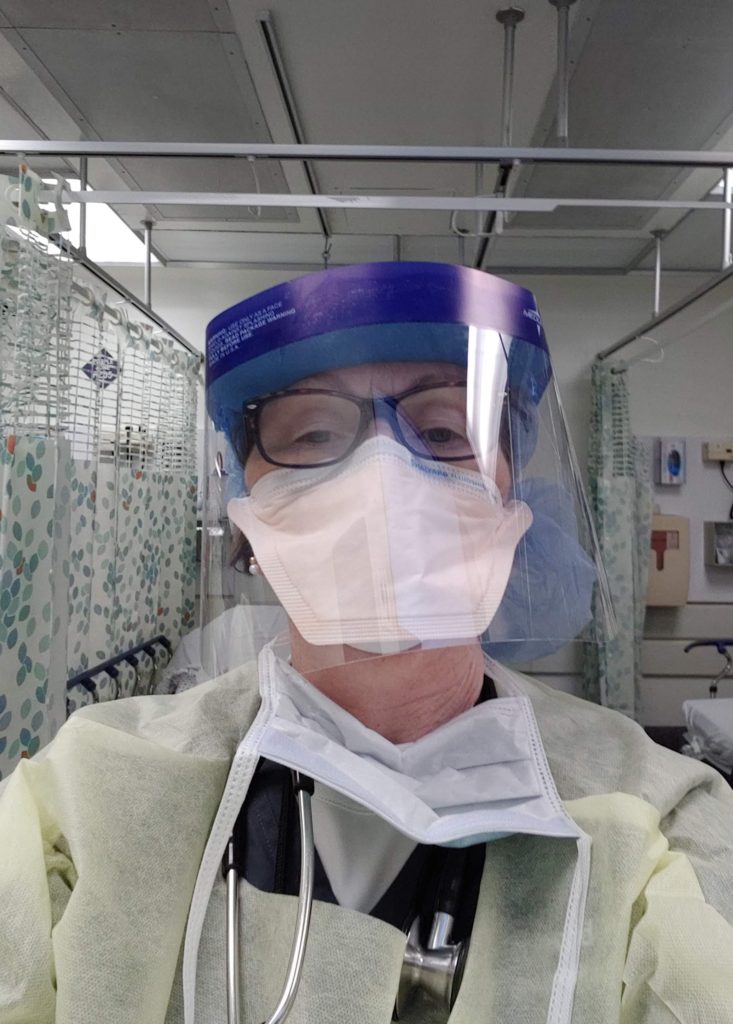
Since 1999, Sister Mary Catherine Redmond has worked as a physician assistant in the emergency department of a small city hospital in the Bronx, part of New York's Health and Hospitals Corporation, which offers service to all who need it, regardless of resources or insurance status. A Preservation Sister, she resides in a Bronx convent with four other members of her congregation.
This spring, when New York became the epicenter of the Covid-19 pandemic, the hospital where Sr. Mary Catherine works - like many in the region - saw a massive influx of cases. Archways Managing Editor Michael Cain spoke with her last week about her experiences in service, the power of prayer and the challenge of connecting with patients and their families at a time when physical contact was fraught with risk.
Archways: How does a Presentation Sister become a physician assistant in the Bronx?
I grew up in Kingston, New York, where I was educated by the Presentation Sisters at St. Mary’s/Kingston Catholic School. I entered the Sisters of the Presentation of the Blessed Virgin Mary on Aug 30, 1987, and made final vows March 23, 1996.
When I entered religious life I was actually an audiologist. I worked at NYU Medical Center for 10 years before I went back to school at the Catholic Medical Center in Queens to become a physician assistant. I did this because I really felt called at that point to provide medical care to the underserved. I never had any idea that I would be working in emergency medicine, but after my studies ended, there was a position open in the emergency department at one of the city hospitals in the Bronx.
As I walked in for the interview, I saw a sign on the side of the building that said: WE TREAT YOUR FAMILY LIKE OUR FAMILY. I saw the place and the people, and I thought: “This is exactly where I’m supposed to be.” There were wonderful, wonderful people providing medical care to those who either didn’t have insurance or were recent immigrants or on Medicaid. I’ve been there for more than 20 years.
Archways: Can you describe your work there since the Covid-19 crisis struck?
Everything happened very quickly with the crisis, especially in the New York City area. It felt like a tidal wave. We were front line in terms of providing medical care. And as the crisis evolved it became clearer and clearer to us that we were dealing with something that was way beyond our control.
In the beginning, when we were working with Covid-positive patients, we were worried about where they had traveled, and what contacts they had, et cetera. Then all of a sudden it was a whole slew of Uber drivers that were very sick, which meant that it was person-to-person contact. And then it evolved even more. Because of the population that we deal with, because it’s the New York City area and families are living in very close quarters, it’s hard to isolate if you are sick. So if one family member was sick, often several family members were sick.
Suddenly, the capacity of the hospital was a concern. It seemed to happen in one week. We didn’t know what we were dealing with. Patients started showing up with all different symptoms, and everyone had Covid. First we were looking for respiratory symptoms and the ground-glass opacities on the chest X-ray. The next thing, it was gastrointestinal symptoms. Then all of a sudden it was “I can’t smell” and “I don’t taste anymore.” They were all Covid.
It was just very scary.
Then there is the fact that – like every institution in the New York City area and probably across the country – we ordinarily would use personal protective equipment for going into the room of one person maybe once a week. For a staff of around 60 people now to have to use that equipment on a daily basis was just beyond the capacity of what we had. So early in the crisis we were wearing our protective wear [which is meant to be used once and discarded] five days in a row, unless there was some sort of compromise.
There was concern about intubating patients because of droplets being aerosolized, so that was a very controlled environment. Only a certain number of people were in the room. Everybody had face shields on.
One of the hardest things for me was not having people even see my face, really, just seeing my eyes. You know, how do you communicate with somebody, how do you reassure somebody with just your eyes? How do they know I’m smiling underneath my mask? Simple things.
And physical touch. Now we had rubber gloves on, we had these gowns on. It was something we had never dreamt of in terms of our own personal expression of care that we offer to people.
Archways: What has been especially difficult during this crisis?
The hardest was having my family say to me, “Please be careful,” and assuring them that I was being careful but knowing I was really at a huge risk. I just lost my mom about two years ago, and having my father say to me, “Mare, please be careful,” and knowing.…
Another hard thing is that I live in the convent with older sisters, so going home and holding the burden that I could potentially infect them was very overwhelming.
And then… the number of deaths. I mean, it was death like we’ve never seen death before. The number of body bags. The last minutes that families had with each other, which we knew were potentially the last they would ever see of their loved one. That was heart-wrenching. And the realization that, when we put people on ventilators – and that was a whole big thing, we needed ventilators, we needed to have a supply – to realize that only 20 percent of the people were ever going to make it off the ventilators was really overwhelming. There were also renal complications. It turned into this multi-organ system failure that was just beyond our control.
But I think that some of the hardest things were also some of the largest blessings. As part of the palliative care team, I had some of the most heart-wrenching and deeply moving and connecting conversations with family members about end of life, about the loss of their loved ones.
One of the nurses, a traveling nurse, suggested that it would be great if at the bottom of the bed we could have a little story of the person. Because then we would all be able to talk to them. Even if they were on ventilators we would be able to know a little bit about them and talk to them. So I spent an afternoon calling the families of all the patients in that unit – which was a makeshift unit for an ICU. I called the families and asked them questions and they talked about their family member. Then I wrote up a little story about them in the first person, like “I love to sail and I’ve been around the world and I also know German in addition to Spanish and English.” We put the story at the bottom of the bed. That was a blessing… just listening to the families talk about their loved ones. I think they felt comforted that someone wanted to know all this information about their family member.
Archways: Have there been other blessings during the crisis?
There were a lot of blessings during that time. I was definitely blessed by the support of my community, of my congregation, the prayer support of many people. I remember once early on in religious life, one of the sisters said to me, “Where one of us is, we all are.” And I would always think, every day, when I walked into the Emergency Department: We are all here. This is where our foundress, Nano Nagle, would be today. Because she went out wherever the need was. And this was where the need was during this crisis.
My prayer life was extremely rich during this time, and that too was a great blessing.
And it was important to have the support of the people that I work with. I remember one day, one of the physician assistants – who had just come back from maternity leave and walked into a pandemic – was on the verge of tears. So I handed her a couple of dollars and said, “Listen, go down the street and get us pizza, and I’ll meet you in the back.” I took care of the patient she had been tending to, and later the physician assistant told me, “Oh, thank you so much, I just needed to get out of here.” Then there were other times that I just sat and cried and other people sat with me.
The palliative care team was an emergency group of people from a number of departments, OB-Gyn and emergency medicine and social work and psychiatry, who all came together because there was just such need. We had so many patients who were so sick that the doctors providing their medical care could not step away to keep in contact with the families. So the palliative care team started reaching out to the families. We met at one o’clock every Monday to Friday and talked about the cases. Several of the people on the team lost family members during that time.
Archways: What will you always remember?
I’ll always remember the names of the patients that died. Its’ like a litany. I still have contact with some of their families. Like one of the mothers, the mother of a 22-year-old. I reached out to her on Mother’s Day and just told her I was praying for her. And there’s another woman whose friend died from Covid. He worked at Walt Disney World, came back to New York when the crisis started and ended up dying – a young guy in his 30s. And his friend, who was so concerned, was really the next of kin for him, because his family was in the Philippines. She’s pregnant and expecting in June, and she said, “I can’t wait until after I have the baby, when I can come and give you a hug.” The intensity of the times made connections that will continue.
Archways: What gives you hope?
I know for sure that an awareness of the health care needs of the poor has been brought into the light. There’s been great insight into the disparity of care.
Archways: Thank you for talking with us, Sister. There are those who say that the Church closed its doors and turned its back on the faithful during the pandemic. Your service, and that of so many other Catholic ministries, is a living rebuttal.
It is interesting that you should say that. It wasn’t that the Church closed. The Church just went to the streets. Whether it was people handing out sandwiches, whether it was people taking care of their neighbors, whether it was people taking care of the sick, the Church went to the streets.
Sr. Mary Catherine Redmond has written three moving blog posts about her experience of the Covid-19 crisis in the Bronx. To read them go to Global Sisters Report.
